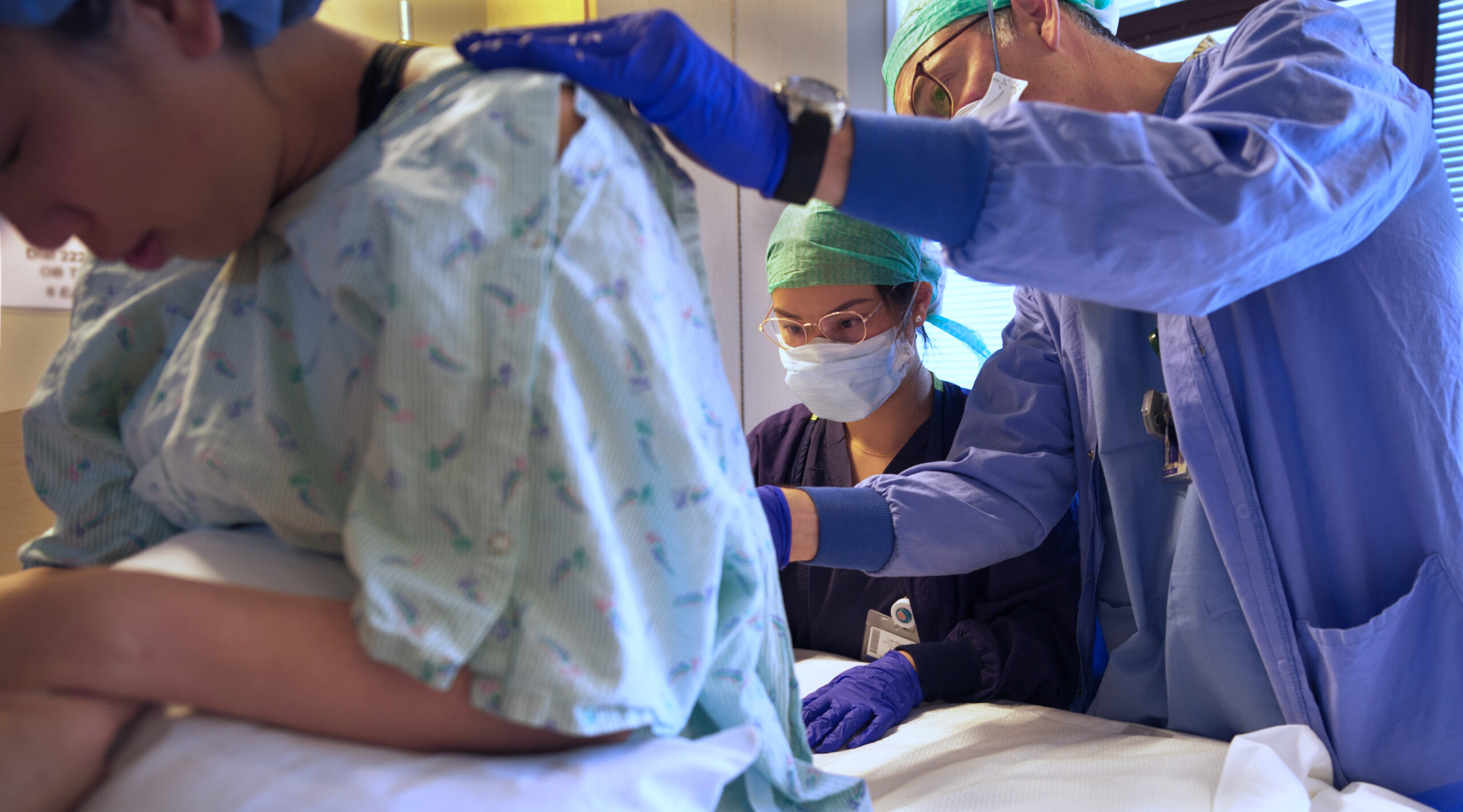
About the Obstetric Anesthesiology Fellowship
The Obstetric Anesthesiology (OBA) Fellowship is a one-year, ACGME-accredited clinical fellowship based at the University of Washington Medical Center – Montlake campus. Our fellows learn and practice excellent clinical care with a focus on anesthetic management of high-risk pregnancy and delivery.
Please refer to UW GME Prospective Residents & Fellows for information about life in Seattle and training at UW.
- Provide professional and superior evidence-based clinical care in a compassionate and individualized manner while respecting each patient’s autonomy and incorporating their self-care goals.
- Train the next generation of obstetric anesthesiologists by continuous active experience-based learning (both for theoretical knowledge and skills) essential to obstetric anesthesiology and geared towards achieving confidence in independent practice.
- Foster the application of evolving concepts in clinical and epidemiological sciences to patient care.
- Stimulate constant self-evaluation and lifelong learning in our trainees.
- Utilize the broad expertise of our faculty to engage in innovative scientific discovery, with ulterior translation and dissemination into everyday practice.
- Engage in community outreach and advocacy at the local, regional, national, and international levels.
- Create an inclusive, rich culture and environment that attracts and retains excellent trainees, faculty and staff from all backgrounds.
Education
Part of becoming an obstetric anesthesiologist is learning to teach obstetric anesthesiology to yourself and others. We follow the SOAP Joint Curriculum Project’s didactic schedule to ensure all important topics and landmark papers are reviewed throughout the year. We expect our fellows to take an active role in the Obstetric Anesthesiology Division’s teaching efforts for residents on their OBA rotations. Fellows will learn to prepare and deliver resident didactics, run simulation sessions, coach residents in point-of-care-ultrasound (POCUS) scanning, and teach and supervise residents performing neuraxial procedures and anesthesia for obstetric surgery.
Our fellows spend two weeks each with the following services:
- Maternal-fetal medicine
- Neonatology
- Transfusion medicine
- Adult congenital heart disease
Clinical experience
The UW Medical Center – Montlake obstetric unit is a tertiary referral center for the entire WWAMI (Washington, Wyoming, Alaska, Montana, and Idaho) region, resulting in an extremely diverse and high-risk patient population. In 2019, UW Medical Center – Montlake had the second highest UHC APR-DRG Severity of Illness Score for all deliveries in the United States. The obstetric unit averages about 2,000 deliveries a year with a 41% cesarean delivery rate and an 85% CSE/epidural rate.
Working closely with other divisions within our hospital, the OBA Division provides an integrated team approach to managing complex cases. Multidisciplinary rounds occur twice daily. Fellows will see antenatal patients on a weekly basis in our fellow-run pre-anesthesia high risk consult clinic and adult congenital cardiac patients on a monthly basis with cardiology and MFM colleagues. High risk patients are discussed twice a month in our Medically Complex Maternal Care Conferences, which occur with our MFM and nursing colleagues as well as other consult services as necessary.
In addition to providing analgesia and anesthesia for labor and delivery, our fellows gain expertise in caring for patients undergoing non-obstetric surgery during pregnancy, fetal surgery, cesarean hysterectomy, cerclage placement, and other surgeries related to pregnancy and delivery.
Medically complicated conditions our fellows may encounter at UW Medical Center – Montlake include:
- Chronic Hypertension, Pre-eclampsia with Severe Features, and HELLP Syndrome
- Abnormal Placentation including Placenta Accreta Spectrum
- Major Cardiac Disease
- Adult Congenital Cardiac Disease
- Pulmonary Hypertension
- Respiratory Diseases
- Endocrine Disorders
- Hematological Disorders
- Transplants
- Extremes of Height and Weight
- Cancer
- Infectious Diseases, including HIV
- Polysubstance Abuse
Research
Research is an integral part of the OBA fellowship. We provide our fellows with protected time for a research project and a case report, which we expect them to present at SOAP.
Our ACGME fellows are represented by the UW House Staff Association Collective Bargaining Agreement. Please refer to UW GME for updated stipend information, insurance and retirement benefits, policies, procedures, and other available resources.
Financial support:
Annual Stipend: The UW OBA Fellowship salary is based on the UW GME schedule and may change from year to year.
Academic Allowance: Subject to available funding, fellows will receive an academic allowance each academic year as “all inclusive” support for their general expenses incurred during their time training.
Other: Fellows receive a fully subsidized bus/light rail pass and are reimbursed for the cost of a Washington State Limited License (or can pay the difference for a full license), ACLS, and NRP.
PTO and leave
Please refer to the UW Resident and Fellow Physician Union – Northwest Contract for institutional PTO and leave allowance, and note that all leave of absence during training is subject to policies set by the American Board of Anesthesiology.
Program Director: Paige M. Keasler, DO
Program Operations Specialist | Fellowship Program Administrator: Ruby Tang
See a complete list of our obstetric anesthesiology faculty and fellows.
SF Match
Our program participates in the nationwide Obstetric Anesthesiology Fellowship Match organized by SF Match. Instructions can be found on the SF Match website and a list of common application and supplementary questions can be found on the SOAP website.
Application documents
Applicants must submit the following documents directly to our program:
- Current Curriculum Vitae
- Obstetric Anesthesiology Fellowship Common Application
- Obstetric Anesthesiology Fellowship Common Application Supplementary Questions
- Three (3) current reference letters, including one from your anesthesiology residency program director or current director
- Current medical license
- Copy of medical school diploma
- ABA Basic Exam Result (if applicable)
- Copy of anesthesia diploma (if applicable)
- All USMLE and/or COMLEX scores
- ECFMG documentation
Please send completed applications and/or questions to our Program Operations Specialist | Fellowship Program Administrator, Ruby Tang.
Important dates
Applications can be submitted starting January 1 and will be accepted until April 30. SF Match’s application opening date varies annually but typically happens in mid-January. Applications are considered on a rolling basis, so we encourage you to submit your application early. The fellowship officially runs from August 1 to July 31 the following year. If needed, we can alter your start date to accommodate the completion of your residency training.
Interviews
Interviews are currently being conducted remotely through Zoom. If you are invited to an interview, we will work together to find a mutually agreeable date and time.